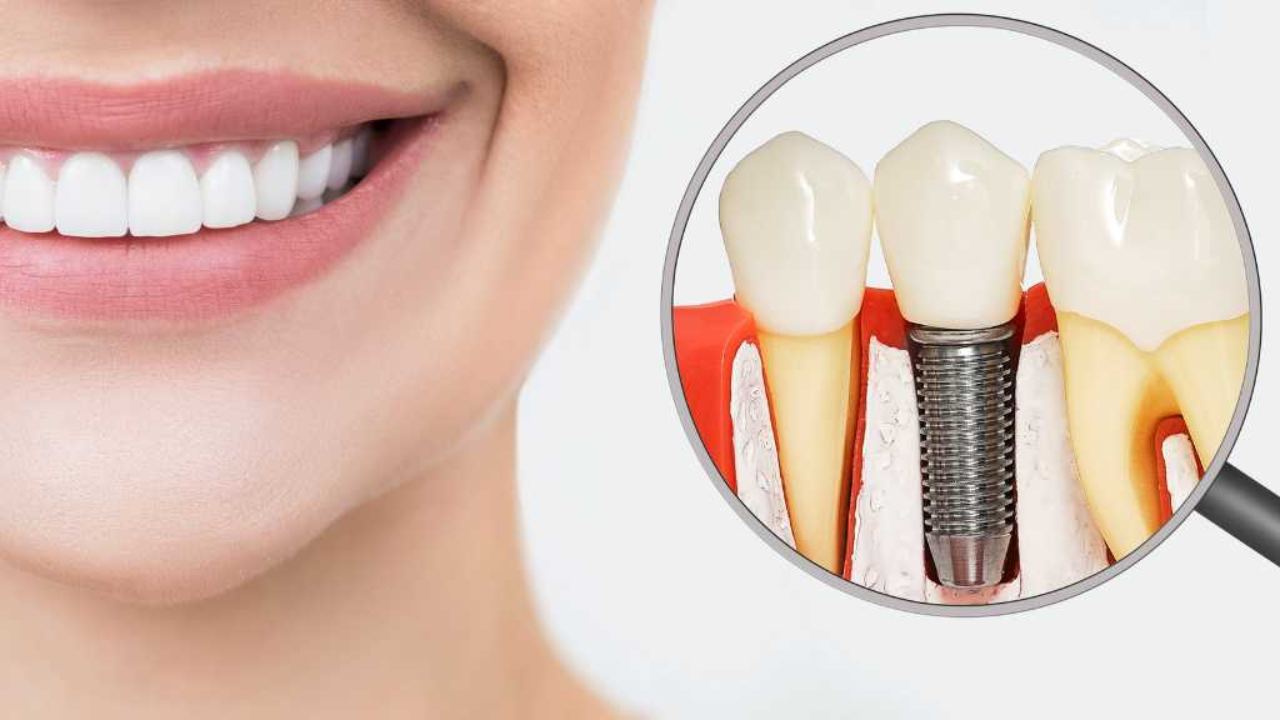
Wisdom teeth are the third set of molars that grow at the very back of your mouth, usually appearing between the ages of 17 and 25. TMJ disorder is a condition affecting the temporomandibular joint — the joint that connects your lower jaw to your skull and controls all jaw movement. These are two different dental issues, but they are often discussed together because they share similar symptoms and can influence each other in ways that are not always obvious.
Understanding what each condition actually is, how they develop, and where they overlap is the first step to figuring out what is going on with your jaw — and what to do about it.
What Is TMJ Disorder?
The temporomandibular joint — commonly called the TMJ — is the hinge connecting your lower jaw to the rest of your skull. You use it constantly: every time you bite, speak, or yawn. When something disrupts this joint or the muscles around it, the result is TMJ disorder (also referred to as TMD).
According to the National Institute of Dental and Craniofacial Research, TMJ disorders affect more than 10 million people in the United States, with women more affected than men. Common signs include:
- Aching pain in the jaw, face, or just in front of the ears
- Clicking, popping, or grinding sounds when moving the jaw
- A bite that suddenly feels off — like your teeth don’t fit together right
- Stiffness or limited range of motion in the jaw
- Occasional jaw lock — where the mouth gets stuck open or won’t close fully
TMJ problems are most commonly triggered by teeth grinding (bruxism), jaw injuries, arthritis, or stress. Wisdom teeth are a less obvious trigger — but they’re not off the hook either.
How Wisdom Teeth Can Affect Your Jaw
Most people develop wisdom teeth — third molars — between the ages of 17 and 25. The problem is that modern jaws often don’t have enough room for them. When a tooth can’t fully emerge, it becomes impacted: trapped beneath the gum, or growing at an angle that puts pressure on everything nearby.
Here’s a simple way to understand the four paths that lead from wisdom teeth to jaw problems — the P.A.I.N. Framework:
P — Pressure on the Joint An impacted wisdom tooth doesn’t sit still. It pushes against surrounding bone, tissue, and neighboring teeth. That pressure can radiate toward the temporomandibular joint, creating strain in the surrounding muscles and contributing to the same kind of inflammation you’d see in TMJ disorder. It’s like a pebble in your shoe — small, but it changes everything about how you move.
A — Alignment Shifts in the Bite As wisdom teeth push against neighboring molars, they can gradually shift how your teeth meet. Even subtle changes in bite alignment force your jaw muscles to compensate — and over time, that uneven load places extra stress on the TMJ. A study published in the Journal of the American Dental Association identified third molar removal as a risk factor for TMJ disorder, suggesting the connection goes beyond coincidence.
I — Inflammation That Spreads Partially erupted wisdom teeth create pockets where bacteria accumulate easily. This leads to pericoronitis — infection and swelling of the gum tissue around the tooth. That inflammation doesn’t always stay local. It can spread to the jaw tissues surrounding the joint, triggering pain and stiffness that looks and feels exactly like a TMJ flare-up.
N — Nerve Tension From Grinding Discomfort from an erupting or impacted wisdom tooth — especially overnight — often triggers unconscious clenching or grinding. Bruxism is one of the most well-documented causes of TMJ disorder. So the wisdom tooth isn’t damaging the joint directly; it’s setting off a chain reaction that puts the joint under sustained pressure.
Most people assume it’s either wisdom teeth or TMJ. The reality is that it’s often one making the other worse — not a clean either/or situation.
Wisdom Teeth and Jaw Lock: What’s the Connection?
Jaw lock is one of the more alarming things that can happen when these two conditions overlap. Your jaw gets stuck, either open or partially closed — and it comes up surprisingly often alongside wisdom tooth problems.
This can happen in two ways. First, significant swelling from an impacted or infected wisdom tooth can physically restrict how far your jaw opens — this is called trismus. Second, if the TMJ itself becomes inflamed, or the small disc inside the joint shifts out of position (which wisdom-tooth-related grinding and pressure can contribute to), locking becomes a direct symptom of joint dysfunction.
If your jaw is locking alongside back-of-mouth pain or visible swelling, that’s not something to wait on. A dental exam can identify whether the root cause is the tooth, the joint, or both working against each other.
TMJ Pain vs. Wisdom Tooth Pain: How to Tell the Difference
The symptoms overlap enough to cause real confusion. Here’s a practical comparison:
- Location: Wisdom tooth pain sits at the very back of the jaw, deep in the gum. TMJ pain radiates from the joint just in front of the ear — and can spread to the face, temples, or neck.
- Sound: Clicking, popping, or grinding sounds when moving the jaw are classic TMJ signs. Wisdom teeth alone rarely cause joint sounds.
- Trigger: If pain flares when you open wide, chew hard food, or yawn, the joint is likely involved. Constant pain with gum swelling at the back points more to wisdom teeth.
- Headaches: Frequent headaches in the temples or behind the eyes are far more associated with TMJ disorder than with wisdom teeth alone.
Without an exam and X-rays, it’s difficult to know for certain — and the wrong assumption leads to the wrong treatment.
What Happens If You Leave It Untreated?
Ignoring wisdom tooth complications rarely ends well. An impacted tooth that keeps pushing against the jaw can lead to crowding, cyst formation, and damage to neighboring teeth. And if it’s quietly feeding into a TMJ problem through grinding or chronic inflammation, the joint damage that accumulates is much harder to reverse than the original issue.
In many cases, removing a problematic wisdom tooth can relieve both the direct symptoms and the downstream pressure it was placing on the jaw. Whether that’s the right move — and whether a separate TMJ treatment plan is also needed — depends entirely on what’s actually going on in your mouth.
If you’re unsure where your jaw pain is coming from, reviewing some common dental implants questions is a good starting point before booking an evaluation.
Frequently Asked Questions
Can wisdom teeth actually cause TMJ disorder?
Not directly. But impacted wisdom teeth can aggravate the joint and trigger grinding, which is a known cause of TMJ disorder.
Will removing wisdom teeth fix my TMJ pain?
Sometimes. If the tooth was causing bite imbalance or grinding, removing it can help. But both issues often need separate treatment.
What does wisdom-tooth-related jaw lock feel like?
Your jaw feels stuck and won’t open or close fully, often with swelling at the back of the mouth. Get it checked — don’t try to force it.
How do I know if jaw clicking is from wisdom teeth or TMJ?
TMJ clicking comes from the joint in front of your ear. Wisdom tooth pain sits at the back of the mouth. An X-ray is the clearest way to tell them apart.
Can TMJ disorder develop after wisdom tooth removal?
Yes, in some cases. Keeping the mouth open during extraction places stress on the TMJ. Proper aftercare reduces the risk.
Is jaw pain from wisdom teeth always a sign of TMJ disorder?
No. Wisdom teeth cause jaw pain on their own without any TMJ disorder present. Only a clinical evaluation can tell the difference.